Ad Support : Nano Technology Netbook Technology News Computer Software
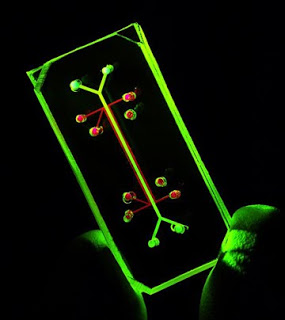
The lung on a chip, shown here, was crafted by combining microfabrication techniques from the computer industry with modern tissue engineering techniques, human cells and a plain old vacuum pump. Photo courtesy of the Wyss Institute for Biologically Inspired Engineering
1. Researchers from the Wyss Institute for Biologically Inspired Engineering at Harvard University, Harvard Medical School and Children’s Hospital Boston have created a device that mimics a living, breathing human lung on a microchip. The device, about the size of a rubber eraser, acts much like a lung in a human body and is made using human lung and blood vessel cells.
The lung-on-a-chip microdevice takes a new approach to tissue engineering by placing two layers of living tissues—the lining of the lung’s air sacs and the blood vessels that surround them—across a porous, flexible boundary. Air is delivered to the lung lining cells, a rich culture medium flows in the capillary channel to mimic blood and cyclic mechanical stretching mimics breathing. The device was created using a novel microfabrication strategy that uses clear rubbery materials. The strategy was pioneered by another Wyss core faculty member, George Whitesides, the Woodford L. and Ann A. Flowers University Professor at Harvard University
potential to use human cells while recapitulating the complex mechanical features and chemical microenvironments of an organ could provide a truly revolutionary paradigm shift in drug discovery
Lung disease accounts for around 400,000 deaths each year in the United States. Lung tissue is difficult to regenerate because it does not generally repair or regenerate beyond the microscopic level. The only current way to replace damaged adult lung tissue is to perform lung transplantation, which is highly susceptible to organ rejection and infection and achieves only 10% to 20% survival at 10 years.
The Yale team says this is an important first step, but a great deal more research must be done to see if fully functional lungs can be regenerated in vitro, implanted and sustained in their functioning. Niklason says that for this technology to be applicable to patients, it is likely that years of research with adult stem cells will be needed to repopulate lung matrices and produce fully functional lungs.
The Yale and Duke University work is in the Science Express.
Because adult lung tissue has limited regeneration capacity, lung transplantation is the primary therapy for severely damaged lungs. To explore whether lung tissue can be regenerated in vitro, we treated lungs from adult rats using a procedure that removes cellular components but leaves behind a scaffold of extracellular matrix that retains the hierarchical branching structures of airways and vasculature. We then used a bioreactor to culture pulmonary epithelium and vascular endothelium on the acellular lung matrix. The seeded epithelium displayed remarkable hierarchical organization within the matrix, and the seeded endothelial cells efficiently repopulated the vascular compartment. In vitro, the mechanical characteristics of the engineered lungs were similar to those of native lung tissue, and when implanted into rats in vivo for short time intervals (45 to 120 min), the engineered lungs participated in gas exchange. Although representing only an initial step toward the ultimate goal of generating fully functional lungs in vitro, these results suggest that repopulation of lung matrix is a viable strategy for lung regeneration
22 pages of supplemental information
If you liked this article, please give it a quick review on Reddit, or StumbleUpon. Thanks
Supporting Advertising
Business Success
How to Make Money
Executive Jobs
Paid Surveys
Thank You

Brian Wang is a Futurist Thought Leader and a popular Science blogger with 1 million readers per month. His blog Nextbigfuture.com is ranked #1 Science News Blog. It covers many disruptive technology and trends including Space, Robotics, Artificial Intelligence, Medicine, Anti-aging Biotechnology, and Nanotechnology.
Known for identifying cutting edge technologies, he is currently a Co-Founder of a startup and fundraiser for high potential early-stage companies. He is the Head of Research for Allocations for deep technology investments and an Angel Investor at Space Angels.
A frequent speaker at corporations, he has been a TEDx speaker, a Singularity University speaker and guest at numerous interviews for radio and podcasts. He is open to public speaking and advising engagements.