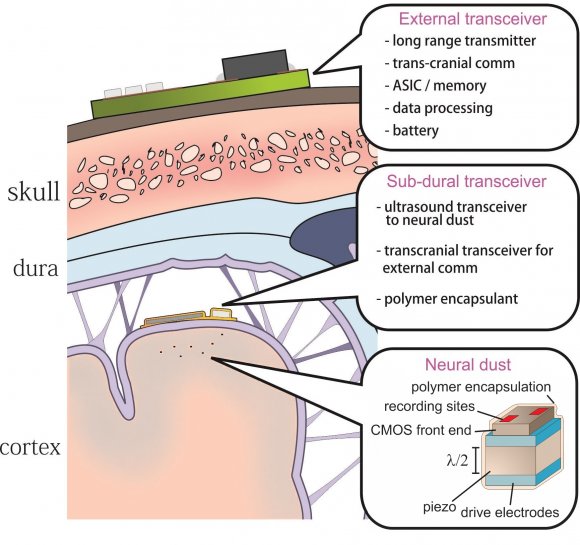
Berkeley engineers have built the first dust-sized, wireless sensors that can be implanted in the body, bringing closer the day when a Fitbit-like device could monitor internal nerves, muscles or organs in real time.
Neural dust researchers have already shrunk them to a 1 millimeter cube – about the size of a large grain of sand – contain a piezoelectric crystal that converts ultrasound vibrations from outside the body into electricity to power a tiny, on-board transistor that is in contact with a nerve or muscle fiber. A voltage spike in the fiber alters the circuit and the vibration of the crystal, which changes the echo detected by the ultrasound receiver, typically the same device that generates the vibrations. The slight change, called backscatter, allows them to determine the voltage.
A major hurdle in brain-machine interfaces (BMI) is the lack of an implantable neural interface system that remains viable for a substantial fraction of a primate lifetime. Recently, sub-mm implantable, wireless electromagnetic (EM) neural interfaces have been demonstrated in an effort to extend system longevity. However, EM systems do not scale down in size well due to the severe inefficiency of coupling radio waves at mm and sub-mm scales.
They propose an alternative wireless power and data telemetry scheme using distributed, ultrasonic backscattering systems to record high frequency (~kHz) neural activity. Such systems will require two fundamental technology innovations:
1) thousands of 10 – 100 um scale, free-floating, independent sensor nodes, or neural dust, that detect and report local extracellular electrophysiological data via ultrasonic backscattering, and
2) a sub-cranial ultrasonic interrogator that establishes power and communication links with the neural dust. We performed the first in vitro experiments which verified that the predicted scaling effects follow theory and that the extreme efficiency of ultrasonic transmission can enable the scaling of the sensing nodes down to 10’s of um.
“I [Michel Maharbiz] think the long-term prospects for neural dust are not only within nerves and the brain, but much broader,“ said Michel Maharbiz, an associate professor of electrical engineering and computer sciences and one of the study’s two main authors. “Having access to in-body telemetry has never been possible because there has been no way to put something supertiny superdeep. But now I can take a speck of nothing and park it next to a nerve or organ, your GI tract or a muscle, and read out the data.“
The UC Berkeley team powered up the passive sensors every 100 microseconds with six 540-nanosecond ultrasound pulses, which gave them a continual, real-time readout. They coated the first-generation motes – 3 millimeters long, 1 millimeter high and 4/5 millimeter thick – with surgical-grade epoxy, but they are currently building motes from biocompatible thin films which would potentially last in the body without degradation for a decade or more.
Neuron – Wireless Recording in the Peripheral Nervous System with Ultrasonic Neural Dust
Highlights
•First in vivo electrophysiological recordings with neural dust motes
•Passive, wireless, and battery-less EMG and ENG recording with mm-scale devices
•Recorded signals transmitted via ultrasonic backscatter from implanted neural dust motes
•Ultrasound as a scalable means of providing wireless power and communication
Summary
The emerging field of bioelectronic medicine seeks methods for deciphering and modulating electrophysiological activity in the body to attain therapeutic effects at target organs. Current approaches to interfacing with peripheral nerves and muscles rely heavily on wires, creating problems for chronic use, while emerging wireless approaches lack the size scalability necessary to interrogate small-diameter nerves. Furthermore, conventional electrode-based technologies lack the capability to record from nerves with high spatial resolution or to record independently from many discrete sites within a nerve bundle. Here, they demonstrate neural dust, a wireless and scalable ultrasonic backscatter system for powering and communicating with implanted bioelectronics. They show that ultrasound is effective at delivering power to mm-scale devices in tissue; likewise, passive, battery-less communication using backscatter enables high-fidelity transmission of electromyogram (EMG) and electroneurogram (ENG) signals from anesthetized rats. These results highlight the potential for an ultrasound-based neural interface system for advancing future bioelectronics-based therapies.
Can get to 8000 times less volume than existing millimeter cubes
While the experiments so far have involved the peripheral nervous system and muscles, the neural dust motes could work equally well in the central nervous system and brain to control prosthetics, the researchers say. Today’s implantable electrodes degrade within 1 to 2 years, and all connect to wires that pass through holes in the skull. Wireless sensors – dozens to a hundred – could be sealed in, avoiding infection and unwanted movement of the electrodes.
“The original goal of the neural dust project was to imagine the next generation of brain-machine interfaces, and to make it a viable clinical technology,” said neuroscience graduate student Ryan Neely. “If a paraplegic wants to control a computer or a robotic arm, you would just implant this electrode in the brain and it would last essentially a lifetime.”
In a paper published online in 2013, the researchers estimated that they could shrink the sensors down to a cube 50 microns on a side – about 2 thousandths of an inch, or half the width of a human hair.
“The beauty is that now, the sensors are small enough to have a good application in the peripheral nervous system, for bladder control or appetite suppression, for example,“ Carmena said. “The technology is not really there yet to get to the 50-micron target size, which we would need for the brain and central nervous system. Once it’s clinically proven, however, neural dust will just replace wire electrodes. This time, once you close up the brain, you’re done.“
The team is working now to miniaturize the device further, find more biocompatible materials and improve the surface transceiver that sends and receives the ultrasounds, ideally using beam-steering technology to focus the sounds waves on individual motes. They are now building little backpacks for rats to hold the ultrasound transceiver that will record data from implanted motes.
They’re also working to expand the motes’ ability to detect non-electrical signals, such as oxygen or hormone levels.
“The vision is to implant these neural dust motes anywhere in the body, and have a patch over the implanted site send ultrasonic waves to wake up and receive necessary information from the motes for the desired therapy you want,” said Dongjin Seo, a graduate student in electrical engineering and computer sciences. “Eventually you would use multiple implants and one patch that would ping each implant individually, or all simultaneously.”
SOURCES- Berkeley, Neuron

Brian Wang is a Futurist Thought Leader and a popular Science blogger with 1 million readers per month. His blog Nextbigfuture.com is ranked #1 Science News Blog. It covers many disruptive technology and trends including Space, Robotics, Artificial Intelligence, Medicine, Anti-aging Biotechnology, and Nanotechnology.
Known for identifying cutting edge technologies, he is currently a Co-Founder of a startup and fundraiser for high potential early-stage companies. He is the Head of Research for Allocations for deep technology investments and an Angel Investor at Space Angels.
A frequent speaker at corporations, he has been a TEDx speaker, a Singularity University speaker and guest at numerous interviews for radio and podcasts. He is open to public speaking and advising engagements.