Circulation and cellular activity were restored in a pig’s brain four hours after its death which challenges long-held assumptions about the timing and irreversible nature of the cessation of some brain functions after death.
This may help doctors find ways to help salvage brain function in stroke patients, or test the efficacy of novel therapies targeting cellular recovery after injury.
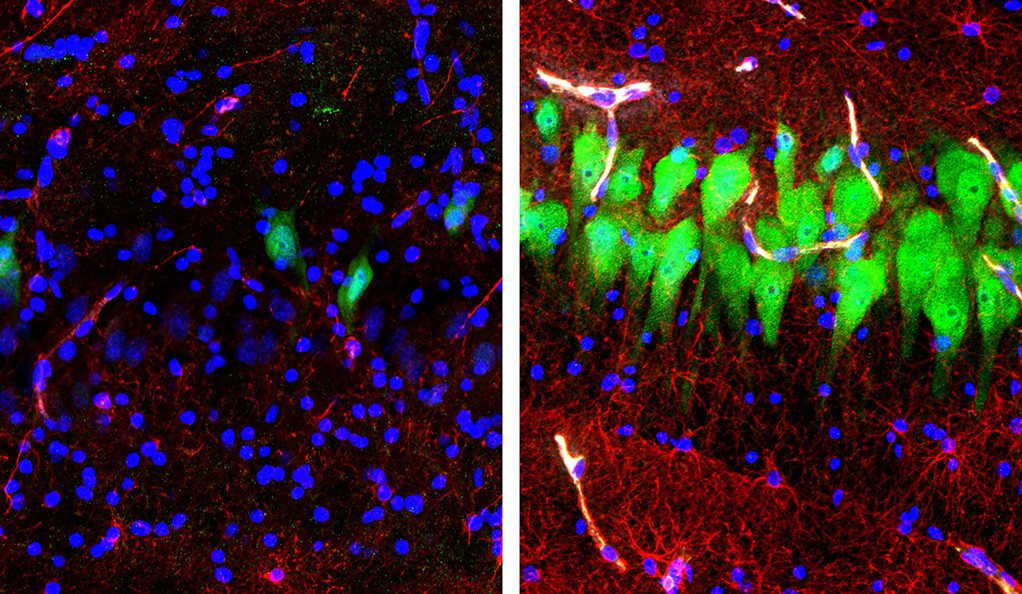
Above -Immunofluorescent stains for neurons (green), astrocytes (red), and cell nuclei (blue) in a region of the hippocampus of a pig’s brain left untreated 10 hours after death (left) or subjected to perfusion with the BrainEx technology. Ten hours postmortem, neurons and astrocytes undergo cellular disintegration unless salvaged by the BrainEx system. (Image credit: Stefano G. Daniele & Zvonimir Vrselja; Sestan Laboratory; Yale School of Medicine)
It is unclear whether this approach can be applied to a recently deceased human brain. The chemical solution used lacks many of the components natively found in human blood, such as the immune system and other blood cells, which makes the experimental system significantly different from normal living conditions. However, the researcher stressed any future study involving human tissue or possible revival of global electrical activity in postmortem animal tissue should be done under strict ethical oversight.
The brain of a postmortem pig obtained from a meatpacking plant was isolated and circulated with a specially designed chemical solution. Many basic cellular functions, once thought to cease seconds or minutes after oxygen and blood flow cease, were observed, the scientists report.
Cellular death within the brain is usually considered to be a swift and irreversible process. Cut off from oxygen and a blood supply, the brain’s electrical activity and signs of awareness disappear within seconds, while energy stores are depleted within minutes. Current understanding maintains that a cascade of injury and death molecules are then activated leading to widespread, irreversible degeneration.
However, researchers in Sestan’s lab, whose research focuses on brain development and evolution, observed that the small tissue samples they worked with routinely showed signs of cellular viability, even when the tissue was harvested multiple hours postmortem. Intrigued, they obtained the brains of pigs processed for food production to study how widespread this postmortem viability might be in the intact brain. Four hours after the pig’s death, they connected the vasculature of the brain to circulate a uniquely formulated solution they developed to preserve brain tissue, utilizing a system they call BrainEx. They found neural cell integrity was preserved, and certain neuronal, glial, and vascular cell functionality was restored.
The new system solves the inability to apply certain techniques to study the structure and function of the intact large mammalian brain — which hinders rigorous investigations into topics like the roots of brain disorders, as well as neuronal connectivity in both healthy and abnormal conditions.
Nature – Restoration of brain circulation and cellular functions hours post-mortem
Abstract
The brains of humans and other mammals are highly vulnerable to interruptions in blood flow and decreases in oxygen levels. Here we describe the restoration and maintenance of microcirculation and molecular and cellular functions of the intact pig brain under ex vivo normothermic conditions up to four hours post-mortem. We have developed an extracorporeal pulsatile-perfusion system and a haemoglobin-based, acellular, non-coagulative, echogenic, and cytoprotective perfusate that promotes recovery from anoxia, reduces reperfusion injury, prevents oedema, and metabolically supports the energy requirements of the brain. With this system, we observed preservation of cytoarchitecture; attenuation of cell death; and restoration of vascular dilatory and glial inflammatory responses, spontaneous synaptic activity, and active cerebral metabolism in the absence of global electrocorticographic activity. These findings demonstrate that under appropriate conditions the isolated, intact large mammalian brain possesses an underappreciated capacity for restoration of microcirculation and molecular and cellular activity after a prolonged post-mortem interval.

Brian Wang is a Futurist Thought Leader and a popular Science blogger with 1 million readers per month. His blog Nextbigfuture.com is ranked #1 Science News Blog. It covers many disruptive technology and trends including Space, Robotics, Artificial Intelligence, Medicine, Anti-aging Biotechnology, and Nanotechnology.
Known for identifying cutting edge technologies, he is currently a Co-Founder of a startup and fundraiser for high potential early-stage companies. He is the Head of Research for Allocations for deep technology investments and an Angel Investor at Space Angels.
A frequent speaker at corporations, he has been a TEDx speaker, a Singularity University speaker and guest at numerous interviews for radio and podcasts. He is open to public speaking and advising engagements.

I’m still waiting for the development of cortical resuscitation. Not that long ago, a person whose heart has stopped or who’s stopped breathing was considered permanently dead. Now we know better. But before we can consider rebooting the electrical activity of the brain, the tissue must first be brought back to a functional state. This is a step in that direction.
Return of Living Dead…
https://www.youtube.com/watch?v=2NhF6zphSx8
..An excellent example of the dangers of creating a science based on easy to observe and understand cause and effect processes while discarding the whole body of evidence at our disposal and the knowledge we have had with us for ions. This is especially true when it comes to the life sciences, like health and death in this case. The views expressed in this article about death are as far as can be from the truth. Here are some links that can provide a better scope:
https://www.youtube.com/watch?v=mMYhgTgE6MU&list=PLtHWLvUowpcR-3F-DT2-eQKGdzSsZvpGa&index=49&t=0s
https://www.youtube.com/watch?v=A1fZT77JFG8
https://www.youtube.com/watch?v=vg8WAv0YT9c&list=PLtHWLvUowpcR-3F-DT2-eQKGdzSsZvpGa&index=48&t=0s
https://www.youtube.com/watch?v=699AFgb8K7A&list=PLtHWLvUowpcR-3F-DT2-eQKGdzSsZvpGa&index=51&t=0s
If we don’t have to rush to keep a person alive then emergency care becomes a lot easier.
Belief is not the same as knowledge. And just because you don’t know how does not make it impossible. When a person is dead his cells goes into a state of suspended animation. After a while bacteria will attack and destroy the body. If the body is preserved I believe it will be possible to resurrect the person days, months and even years later. Arise Lazarus.
This excerpt from Greg Egan’s “Distress” comes to mind:
https://www.gregegan.net/DISTRESS/Excerpt/DistressExcerpt.html
Or as Stephen King in Pet Sematary said: “sometimes, dead is better”.
My dear departed aunt Martha was a dear woman, and very talkative, until her stroke. It was tragic. She did not speak a word the rest of her life, ten years or so. Her gait was affected too, but she could get around if the slope was not steep.
If she could have spoken just a few words, it would have been a huge blessing. You don’t realize how much even a little bit means, till you have none at all.
OMG the “walking dead” isn’t fantasy
You do still have reperfusion injury in brain. Yea, not quite what it is in myocardium but still not something you want.
The anoxic injury patterns are actually pretty similar, histologically. Within a few hours, you’ll start seeing neutrophilic infiltrate which will extend up to a week. After that, macrophages and fibrosis starts getting laid down.
Will it work on politicians or has it already been too long for them?
Readling’s & Bellmore’s comments appreciated, and appear accurate to me although I’m not an authority in these biomed fields.
Ischemia/reperfusion injury is the major issue here. Each organ or even tissue in the organism may cope with different manifestations of I/R influenced by factors specific to metabolism of those cells. Heart, liver, kidneys, lung to name a few…would all have differences in mechanisms of injuries and the sequence & scale of events.
The I/R challenges for the ongoing practice of organ transplantation are worth thinking about. There have been publications in that field calling for research in techniques of organ reconditioning. This work discussed here, may contribute to that conversation as well.
For anyone interested in more reading – [from the Nature paper & then a tweet]
#BrainEx
nature.com/articles/s4158…
fr.Suppl.Table 2, “Perfusate”
substrates-glucose, pyruvate
cytoprotective agents-2-Iminobiotin,Necrostatin-1,Disufenton sodium(NXY-059),Sodium 3-Hydroxybutyric Acid,Glutathione Monoethyl Ester,Minocycline,Lamotrigine,QVD-Oph,Methylene Blue
It’s a long way from keeping something alive and it being as serviceable as it was pre death
This solution may turn out to be even more useful in heart attack patients, since heart surgery is less problematic than brain. Reperfusion injury isn’t the issue it is for the brain, but who knows? Heck, for the heart, all the major blood vessels are right there on the surface! Not only that, catheterization which is regularly done on heart patients, could be an option.
If surgery could clear the blockage in a coronary artery, the solution might allow the surgeon to save the heart muscle that has been deprived of blood flow. Normally, the tissue dies, and is replaced by scar tissue.
If this is ten hours at between body, and room temperature, it may be a very big deal. If it’s ten hours a few degrees above freezing, not so much.
If stroke victims can have damaged portions of their brains reperfused with this solution, and then transitioned back to their own blood, functionality might be more, or less restored. That would truly revolutionize the treatment of strokes.
Most strokes are caused by either a burst blood vessel, or a clot,embolism(air bubble), or some other debris blocking a blood vessel. In the case of a clot, an enzyme, TPA(tissue plasminogen activator) may dissolve the clot, restoring circulation. It other cases, surgery would likely be needed to restore circulation. The problem with brain surgery is that unless the region affected by the stroke is near the surface of the brain, accessing it may cause more damage than the stroke. Unlike most organs, you can’t just suture the brain back together, and have it function properly.
This solution must somehow avoid reperfusion injury. When the brain is deprived of oxygen, there is initially little damage done, but upon the return of oxygen to the brain, there is a cascade of events that cause irreversible damage. If the victim has been kept very cold, as in drowning victims stuck below the ice of a frozen lake, reperfusion injury may be avoided. If a loved one has a massive stroke, the best first aid treatment might be to pack their entire body, particularly the head in ice.
I am ready for what’s coming. Got a couple of spears in my backyard.
You know, this is NOT actually all that new. What happens when the brain runs out of energy is that the membrane ion pumps shut down, leading the the capillaries spasming shut, (The brain’s capillaries are a bit different in that respect.) which makes reperfusing the brain very difficult. Aside from that, there isn’t a lot of immediate damage.
This has been known for decades in cryonics circles, which is why the initial perfusion protocol always involves a calcium channel blocker, and a perfusion solution which is designed to mimic the normal cell interior electrolyte balance, rather than normal blood electrolytes.
The brain’s death actually takes many hours, and is a gradual step by step process, NOT some kind of throwing a switch and, bang, you’re dead, thing. One cell system after another decays or self-destructs.
The brains being discussed here are pretty badly damaged at that point, though they’re not entirely dead in every respect. It would take some hefty detail work, maybe even Drexler’s molecular nanotech, to get them fully functional again.