For the first time, researchers have demonstrated a means of controlling cell functions with a physical, rather than chemical, signal. Immune cells coated with nanoparticles take up calcium in the presence of a magnetic field. Each nanoparticle measures approximately 30 nanometers in diameter.
In this image, yellow cells are taking up calcium in response to a localized magnetic field. Cells that are farther away from the field are shown in purple and do not take up calcium. Credit: Donald Ingber, Harvard Medical School
Using a magnetic field to pull together tiny beads targeted to particular cell receptors, Harvard researchers made cells take up calcium, and then stop, then take it up again.
This is another important step to cellular and molecular control to enable nanomedicine
Ingber’s group demonstrated its method for biomagnetic control using a type of immune-system cell that mediates allergic reactions.
Targeted nanoparticles with iron oxide cores were used to mimic antigens in vitro. Each is attached to a molecule that in turn can attach to a single receptor on an immune cell. When Ingber exposes cells bound with these particles to a weak magnetic field, the nanoparticles become magnetic and draw together, pulling the attached cell receptors into clusters. This causes the cells to take in calcium. (In the body, this would initiate a chain of events that leads the cells to release histamine.) When the magnetic field is turned off, the particles are no longer attracted to each other, the receptors move apart, and the influx of calcium stops.
“It’s not the chemistry; it’s the proximity” that activates such receptors, says Ingber.
The approach could have a far-reaching impact, as many important cell receptors are activated in a similar way and might be controlled using Ingber’s method.
“In recent years, there has been a realization that physical events, not just chemical events, are important” to cell function, says Shu Chien, a bioengineer at the University of California, San Diego. Researchers have probed the effects of physical forces on cells by, for example, squishing them between plates or pulling probes across their surfaces. But none of these techniques work at as fine a level of control as Ingber’s magnetic beads, which act on single biomolecules.
Many drugs, from anticancer antibodies to hormones, work by activating cell receptors. Once a hormone is in the blood, however, there’s no turning it on or off. “This shows that you can turn on and off the signal, and that you can do it instantly,” says Christopher Chen, a bioengineer at the University of Pennsylvania. “That’s something that’s hard to do, for example, with an antibody.”
Ingber has many ideas for devices that might integrate his method of cellular control. Magnetic pacemakers could use cells instead of electrodes to send electrical pulses to the heart. Implantable drug factories might contain many groups of cells, each of which makes a different drug when activated by a magnetic signal. Biomagnetic control might lead to computers that can take advantage of cells’ processing power. “Cells do complex things like image processing so much better than computers,” says Ingber. Ingber, who began the project in response to a call by the Defense Advanced Research Projects Agency for new cell-machine interfaces, acknowledges that his work is in its early stages. In fifty years, however, he expects that there will be devices that “seamlessly interface between living cells and machines.”
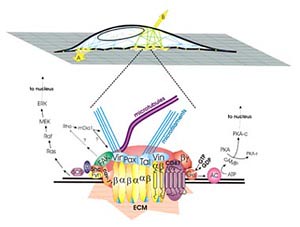
Picture of a cell and expanded view of a cell receptor
FURTHER READING
Harvard Institute for Biologically Inspired Engineering.

Brian Wang is a Futurist Thought Leader and a popular Science blogger with 1 million readers per month. His blog Nextbigfuture.com is ranked #1 Science News Blog. It covers many disruptive technology and trends including Space, Robotics, Artificial Intelligence, Medicine, Anti-aging Biotechnology, and Nanotechnology.
Known for identifying cutting edge technologies, he is currently a Co-Founder of a startup and fundraiser for high potential early-stage companies. He is the Head of Research for Allocations for deep technology investments and an Angel Investor at Space Angels.
A frequent speaker at corporations, he has been a TEDx speaker, a Singularity University speaker and guest at numerous interviews for radio and podcasts. He is open to public speaking and advising engagements.

