Scientists at the Biodesign Institute at Arizona State University have turned to a promising field called DNA nanotechnology to make an entirely new class of synthetic vaccines. They developed the first vaccine complex that could be delivered safely and effectively by piggybacking onto self-assembled, three-dimensional DNA nanostructures. They developed an immune response in mice that was robust immune response up to 9-fold higher than with antigen and adjuvant alone.
Safe and effective vaccines offer the best intervention for disease control. One strategy to maximize vaccine immunogenicity without compromising safety is to rationally design molecular complexes that mimic the natural structure of immunogenic microbes but without the disease-causing components. Here we use highly programmable DNA nanostructures as platforms to assemble a model antigen and CpG adjuvants together into nanoscale complexes with precise control of the valency and spatial arrangement of each element. Our results from immunized mice show that compared to a mixture of antigen and CpG molecules, the assembled antigen-adjuvant-DNA complexes induce strong and long-lasting antibody responses against the antigen without stimulating a reaction to the DNA nanostructure itself. This result demonstrates the potential of DNA nanostructures to serve as general platforms for the rational design and construction of a variety of vaccines.
Nanoletters – A DNA Nanostructure Platform for Directed Assembly of Synthetic Vaccines
“When Hao treated DNA not as a genetic material, but as a scaffolding material, that made me think of possible applications in immunology,” said Chang, an associate professor in the School of Life Sciences and a researcher in the Biodesign Institute’s Center for Infectious Diseases and Vaccinology. “This provided a great opportunity to try to use these DNA scaffolds to make a synthetic vaccine.”
“The major concern was: Is it safe? We wanted to mimic the assembly of molecules that can trigger a safe and powerful immune response in the body. As Hao’s team has developed a variety of interesting DNA nanostructures during the past few years, we have been collaborating more and more with a goal to further explore some promising human health applications of this technology.”
The state-of-the-art in vaccine development relies on genetic engineering to assemble immune system stimulating proteins into virus-like particles (VLPs) that mimic the structure of natural viruses—minus the harmful genetic components that cause disease.
DNA nanotechnology, where the molecule of life can be assembled into 2-D and 3-D shapes, has an advantage of being a programmable system that can precisely organize molecules to mimic the actions of natural molecules in the body.
“We wanted to test several different sizes and shapes of DNA nanostructures and attach molecules to them to see if they could trigger an immune response,” said Yan, the Milton D. Glick Distinguished Chair in the Department of Chemistry and Biochemistry and researcher in Biodesign’s Center for Single Molecule Biophysics. With their biomimicry approach, the vaccine complexes they tested closely resembled natural viral particles in size and shape.
As proof of concept, they tethered onto separate pyramid-shaped and branched DNA structures a model immune stimulating protein called streptavidin (STV) and immune response boosting compound called an adjuvant (CpG oligo-deoxynucletides) to make their synthetic vaccine complexes.
First, the group had to prove that the target cells could gobble the nanostructures up. By attaching a light-emitting tracer molecule to the nanostructures, they found the nanostructures residing comfortably within the appropriate compartment of the cells and stable for several hours—-long enough to set in motion an immune cascade.
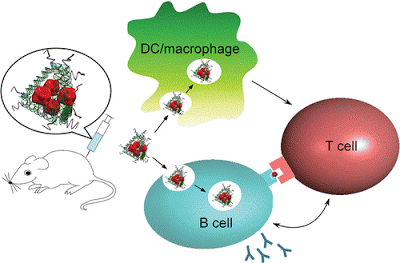
Next, in a mouse challenge, they targeted the delivery of their vaccine cargo to cells that are first responders in initiating an effective immune response, coordinating interaction of important components, such as: antigen presenting cells, including macrophages, dendritic cells and B cells. After the cargo is internalized in the cell, they are processed and “displayed” on the cell surface to T cells, white blood cells that play a central role in triggering a protective immune response. The T cells, in turn, assist B cells with producing antibodies against a target antigen.
To properly test all variables, they injected: 1) the full vaccine complex 2) STV (antigen) alone 3) the CpG (adjuvant) mixed with STV.
Over the course of 70 days, the group found that mice immunized with the full vaccine complex developed a more robust immune response up to 9-fold higher than the CpG mixed with STV. The pyramid (tetrahedral) shaped structure generated the greatest immune response. Not only was immune response to the vaccine complex specific and effective, but also safe, as the research team showed, using two independent methods, that no immune response triggered from introducing the DNA platform alone.
“We were very pleased,” said Chang. “It was so nice to see the results as we predicted. Many times in biology we don’t see that.”
With the ability to target specific immune cells to generate a response, the team is excited about the prospects of this new platform. They envision applications where they could develop vaccines that require multiple components, or customize their targets to tailor the immune response.
Furthermore, there is the potential to develop targeted therapeutics in a similar manner as some of the new generation of cancer drugs.
Overall, though the field of DNA is still young, the research is advancing at a breakneck pace toward translational science that is making an impact on health care, electronics, and other applications.
While Chang and Yan agree that there is still much room to explore the manipulation and optimization of the nanotechnology, it also holds great promise. “With this proof of concept, the range of antigens that we could use for synthetic vaccine develop is really unlimited,” said Chang.
15 pages of supporting material
If you liked this article, please give it a quick review on ycombinator or StumbleUpon. Thanks

Brian Wang is a Futurist Thought Leader and a popular Science blogger with 1 million readers per month. His blog Nextbigfuture.com is ranked #1 Science News Blog. It covers many disruptive technology and trends including Space, Robotics, Artificial Intelligence, Medicine, Anti-aging Biotechnology, and Nanotechnology.
Known for identifying cutting edge technologies, he is currently a Co-Founder of a startup and fundraiser for high potential early-stage companies. He is the Head of Research for Allocations for deep technology investments and an Angel Investor at Space Angels.
A frequent speaker at corporations, he has been a TEDx speaker, a Singularity University speaker and guest at numerous interviews for radio and podcasts. He is open to public speaking and advising engagements.